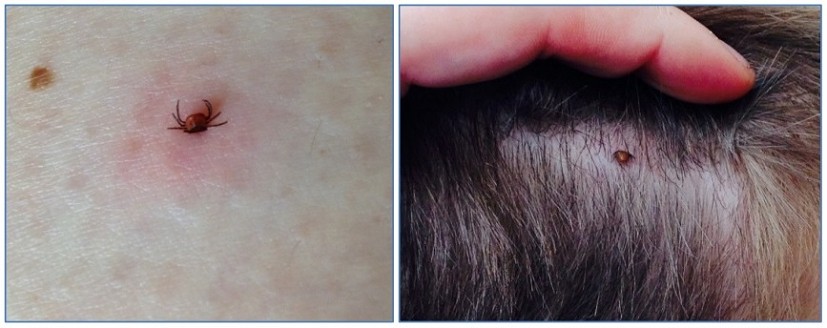
How To Avoid Ticks and Lyme Disease
Ticks have arguably the most dangerous bite to humans of any species in the British Isles. Our warming climate will only make things worse as ticks become able to breed all the way through winter, and it is now not uncommon to find ticks on dogs in the winter months. Walkers and climbers are at particular risk too. Why is such a small creature so scary? Two words: Lyme disease.
Ticks are arachnids, part of the spider family. A tick may be completely harmless but many carry different diseases, from Tick-Borne Encephalitis and Rocky Mountain Spotted Tick Fever to Babesia, Q fever and Louping-ill. More recently one has been discovered in the New Forest which can cause a fatal allergic reaction to red meat. However the most well known is Lyme disease, caused by bacteria of the Borrelia type. Until recently Lyme was thought to be an import from our American cousins, but it is far more likely that we exported it to America as there is evidence of Lyme disease in 3000 year old skeletons in the Orkneys, and Otzi the Iceman in Austria was also found to have it.
At the moment around 2500 cases of Lyme disease are reported each year in the UK and it is now reportable under RIDDOR; however doctors are not obliged to report it unless it is work related, so there may be many other cases out there. One expert entomologist, Ian Burgess, Director for Insect Research and Development in Cambridge, thinks that the true figure is more like 35,000.
Lyme disease hot spots:
Although some areas in particular are flagged up as being higher risk, among them the Lake District, the New Forest, Hampshire, the North York Moors, the Scottish Highlands and Exmoor, in truth wherever there are ticks there is a risk of infection - even in urban parks such as London's Richmond Park.
Lyme disease is hard to spot. Here's why:
1) Many people who develop the symptoms are not aware that they have been bitten by a tick in the first place.
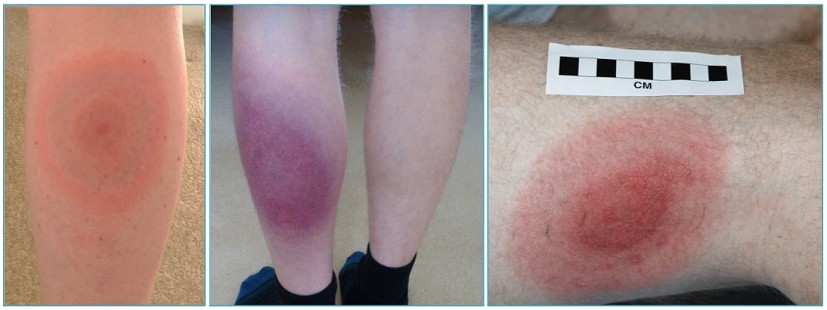
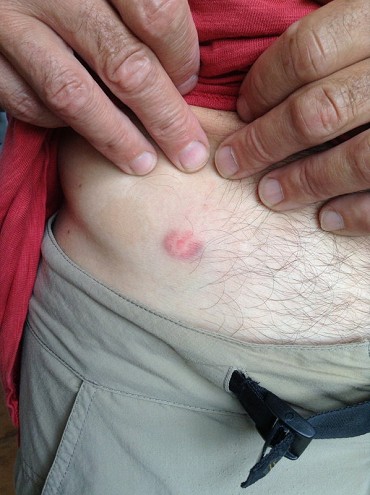
2) The one sure sign of having Lyme disease is the 'bulls eye' rash (erythema migrans). In a perverted sort of way, you are actually lucky if you develop this as it confirms that you have Lyme disease. However less than 40% of people who have Lyme disease had a bulls eye rash to confirm.
3) The disease is still relatively little-known among medical practitioners in Britain, even in areas of high risk. As a result it is not uncommon for doctors to refuse to accept that Lyme exists in the UK, while others might insist that you cannot possibly have it unless you also have the textbook bull's eye rash. Anecdotally, friends of ours have met with both of these reactions.
4) The blood tests for Lyme disease may not show any sign until the body produces some antibodies to the disease, by which time it may already have taken hold.
5) The signs and symptoms are so variable, and may take different lengths of time to appear, that people may not associate them with a tick bite many months ago. There is disagreement from experts on the incubation period for Lyme disease, with quotes of anything from three days to up to six months.
Signs and symptoms of Lyme Disease:
- Headaches
- Aching joints
- Stiff neck
- All over itching
- Swollen lymph glands
- Flu-like symptoms
- Irreversible arthritis of the joints
- Heart arrhythmia and palpitations
- Photo-sensitivity (dislike of bright lights)
- Shooting pains
- Eye inflammation
- Blindness
- Exhaustion and apathy (it's thought by some many cases of rural Chronic Fatigue Syndrome may actually be undiagnosed Lyme disease)
So as you can see there are many signs and symptoms, and different people get different ones. This may be because Lyme disease is thought to supress the immune system, so if someone is exposed to a certain virus whilst being infected with Lyme disease, those are the symptoms which develop.

How to lessen the likelihood of catching Lyme disease? The only sure answer is not to get bitten:
- Avoid animal pathways through undergrowth as ticks 'quest' on host pathways (they stand up on their hind legs and use their front legs to grab hold of passing animals).
- Wear trousers and long-sleeved tops if going through that sort of vegetation.
- Tuck trousers into socks in risky areas (not the in-fashion at present, but it could save you a lot of misery!).
- Wear light coloured trousers so you can see the ticks more easily.
- Woolly and furry fabrics are easier for ticks to cling on to so these are best avoided.
- Insect repellent applied around the legs can help prevent ticks taking hold. DEET-based repellents are thought most effective.
- If a tick is attached, remove it promptly with a suitable device designed expressly for the purpose (see below).
Removing a tick
It is thought that so long as you don't distress a tick it is reasonably safe for about the first 24 hours of attachment, because to begin with it just feeds. Only when it has digested and taken on board food (your blood) does it start to get rid of waste products (including any disease it carries) into your bloodstream.
Dos and don'ts of tick removal:
- Do use a mechanical device such as a tick twister or a tick lasso. These devices are able to slip between the tick's head and jaws (the weakest section of the tick is between body and head and if you just pull on the body, you will end up leaving the tick's head and jaws still embedded into your skin). Personally I would not use a tick card as I have never had any success in removing ticks with it (and with owning dogs, I have had plenty of practice).
- Do go to a doctor if you have any flu like symptoms or other strange symptoms in the weeks after a tick bite or any symptoms which keep reoccurring or not going away.
- Do not use anything chemical to remove the tick. Folklore suggests any number of ways to remove ticks: a cotton bud soaked in soap and water; surgical or methylated spirits; a direct dose of insect repellent onto the tick; smothering it in gel, toothpaste or butter; burning it with a cigarette lighter or the end of a cigarette. Yes, all these methods will remove the tick but unfortunately they also distress it, at which point it will instantly regurgitate its stomach contents into your bloodstream, so injecting you with any disease it carries.
- Do not try to pull the tick off with your fingers or tweezers. The weakest joint on the tick is between the head and body. By pulling you will leave the head and jaws embedded in the skin and remove only the body. This means the infection will still be attached to you. Also by squeezing the body you will be forcing the stomach contents into yourself. Not a good result!
- Do not be fobbed off by doctors telling you that we dont have Lyme disease in the UK, or that you personally cannot have it because you aren't exhibiting the classic bulls eye rash. Remember that only a proportion of people with Lyme disease actually develop this rash, and any rash around the tick bite could be a sign of infection.
On a positive note, there is now a vaccination for dogs against Lyme disease which suggests one may become available to humans in the next few years.
As a postscript, (and a more negative note) there is also a belief that ticks are not the only way that Lyme Disease is spread. There is a theory, as yet just a theory, that mosquitos and midges may also spread the disease.
- For more info on Lyme disease Public Health England have produced a leaflet - see here
- Lyme Disease Action (LDA) is a charity that works towards the prevention and treatment of Lyme disease and associated tick borne diseases - see here
About Helen Howe
Helen runs Snowdonia First Aid with her husband Steve.
Each have over twenty years of Scottish winters and are qualified Winter and International Mountain Leaders. They run Outdoor First Aid courses and Mountain Leader Training and Assessments as well as mountain and hill skills courses. This winter Helen and Steve are running Winter Skills courses both in Snowdonia and Scotland.
Helen is also a qualified Mountain Rescue Dog handler who has trained three SARDA dogs. Both she and Steve are active members of Llanberis Mountain Rescue Team and have served on the Medical and Training Sub committees running some of the team's winter training.